Summary
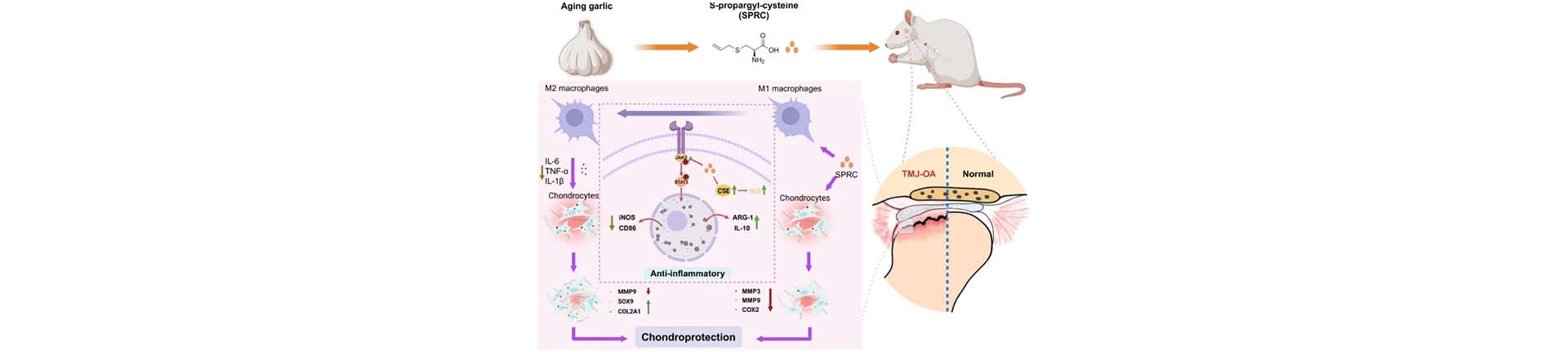
This study investigates the therapeutic effects of S-propargyl-cysteine (SPRC), a hydrogen sulfide (H₂S) donor, in temporomandibular joint osteoarthritis (TMJ-OA), a degenerative condition characterized by synovial inflammation and cartilage destruction. Using both a monosodium iodoacetate (MIA)-induced rat model of TMJ-OA and lipopolysaccharide (LPS)-stimulated RAW264.7 macrophages, SPRC was shown to ameliorate joint damage by modulating macrophage polarization. Specifically, SPRC suppressed pro-inflammatory M1 macrophage activity while promoting an anti-inflammatory M2 phenotype, mediated through inhibition of the JAK2/STAT3 signaling pathway. This shift resulted in decreased expression of inflammatory mediators such as TNF-α, IL-6, and iNOS.
In vivo, SPRC administration improved subchondral bone structure and cartilage integrity, as confirmed by micro-CT and histological analyses. In vitro, SPRC not only directly attenuated inflammatory responses in macrophages but also, through macrophage-chondrocyte co-culture experiments, preserved chondrocyte function and extracellular matrix (ECM) homeostasis. The study identifies JAK2/STAT3 inhibition as a central mechanism underlying SPRC’s anti-inflammatory and cartilage-protective effects. These results highlight SPRC as a promising disease-modifying agent for TMJ-OA, acting through immunomodulation of the synovial microenvironment and support for cartilage regeneration.
W. Cai et al., “S-propargyl-cysteine attenuates temporomandibular joint osteoarthritis by regulating macrophage polarization via Inhibition of JAK/STAT signaling,” Mol Med, vol. 31, no. 1, p. 128, Apr. 2025, doi: 10.1186/s10020-025-01186-6